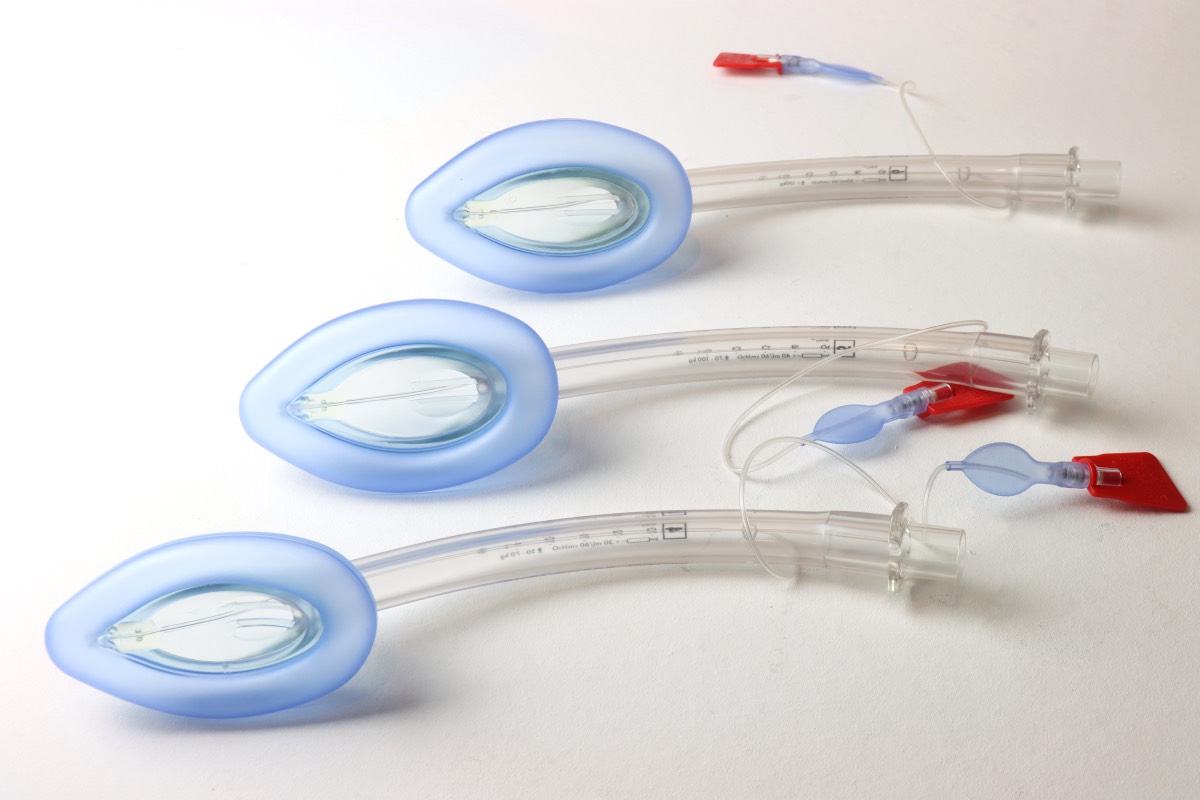
The laryngeal mask airway (LMA) is a widely used supraglottic airway device that serves as an alternative to endotracheal intubation during general anesthesia. Its effectiveness depends on the formation of an adequate seal between the inflatable cuff and the surrounding periglottic tissues, preventing gas leakage during ventilation and reducing the risk of gastric insufflation or aspiration. Because LMAs are frequently used for controlled ventilation as well as airway protection in spontaneous ventilation, testing that the seal is secure is an essential step after insertion. An insufficient seal may lead to inadequate oxygen and/or anesthetic delivery, as well as gastric insufflation. Several clinical methods exist to assess seal integrity, but the most commonly used approach is the measurement of oropharyngeal leak pressure (OLP), also referred to as airway leak pressure, which provides an estimate of the pressure at which gas begins to escape around the device cuff (1).
Following insertion and cuff inflation, clinicians typically evaluate the seal of an LMA by measuring the oropharyngeal leak pressure. This is commonly performed by closing the adjustable pressure-limiting (APL) valve of the anesthesia circuit while maintaining a constant fresh gas flow, allowing airway pressure to gradually rise. As pressure increases, gas will eventually leak around the cuff if the seal limit is reached. The presence of a leak may be detected by hearing gas escaping at the patient’s mouth or observing a stabilization of airway pressure on the anesthesia monitor. The airway pressure at which the leak is first observed represents the OLP and indicates the adequacy of laryngeal mask airway (LMA) positioning and sealing capacity. In many clinical settings, leak pressures of approximately 20–30 cm H₂O are considered sufficient to support positive pressure ventilation during routine anesthetic management (1).
Different generations of supraglottic airway devices have varying sealing capabilities. Second-generation LMAs, such as the ProSeal LMA and the LMA Supreme, have improved cuff geometry and additional features like gastric drainage channels to enhance safety and sealing performance. Clinical studies comparing these devices with earlier LMAs have demonstrated higher oropharyngeal leak pressures, which suggests improved ventilation efficiency and a reduced risk of gastric insufflation during positive pressure ventilation. A meta-analysis evaluating the ProSeal LMA reported significantly higher leak pressures compared to other supraglottic devices, which reinforces the importance of device design in achieving an effective airway seal (3).
Testing the LMA seal is important, especially when positive pressure ventilation is required, such as during laparoscopic procedures or in patients with decreased lung compliance. If the measured leak pressure is low, clinicians may attempt corrective measures, such as repositioning the device, adjusting the position of the head and neck, reinflating the cuff, or placing an LMA of a different size. Failure to obtain an adequate seal may necessitate conversion to endotracheal intubation to ensure safe airway management.
In addition to leak pressure testing, clinicians can evaluate seal integrity by observing tidal volume delivery and the absence of audible leaks during ventilation. Modern studies examining supraglottic airway devices emphasize that a reliable airway seal supports ventilation and improves patient safety by minimizing gastric insufflation and potential aspiration (4). Consequently, routine testing of the LMA seal immediately after placement is considered a fundamental component of safe anesthetic practice. By confirming adequate sealing pressure, anesthesia providers can ensure the device is functioning effectively and will maintain ventilation throughout the procedure.
References
1. Buckham M, Brooker M, Brimacombe J, Keller C. A comparison of the reinforced and standard laryngeal mask airway: ease of insertion and the influence of head and neck position on oropharyngeal leak pressure and intracuff pressure. Anaesth Intensive Care. 1999;27(6):628-631. doi:10.1177/0310057X9902700612
2. Saraswat N, Kumar A, Mishra A, Gupta A, Saurabh G, Srivastava U. The comparison of Proseal laryngeal mask airway and endotracheal tube in patients undergoing laparoscopic surgeries under general anaesthesia. Indian J Anaesth. 2011;55(2):129-134. doi:10.4103/0019-5049.79891
3. Maitra S, Baidya DK, Arora MK, Bhattacharjee S, Khanna P. Laryngeal mask airway ProSeal provides higher oropharyngeal leak pressure than i-gel in adult patients under general anesthesia: a meta-analysis. J Clin Anesth. 2016;33:298-305. doi:10.1016/j.jclinane.2016.04.020
4. van Zundert AAJ, Wyssusek KH, Pelecanos A, Roets M, Kumar CM. A prospective randomized comparison of airway seal using the novel vision-guided insertion of LMA-Supreme® and LMA-Protector®. J Clin Monit Comput. 2020;34(2):285-294. doi:10.1007/s10877-019-00301-3