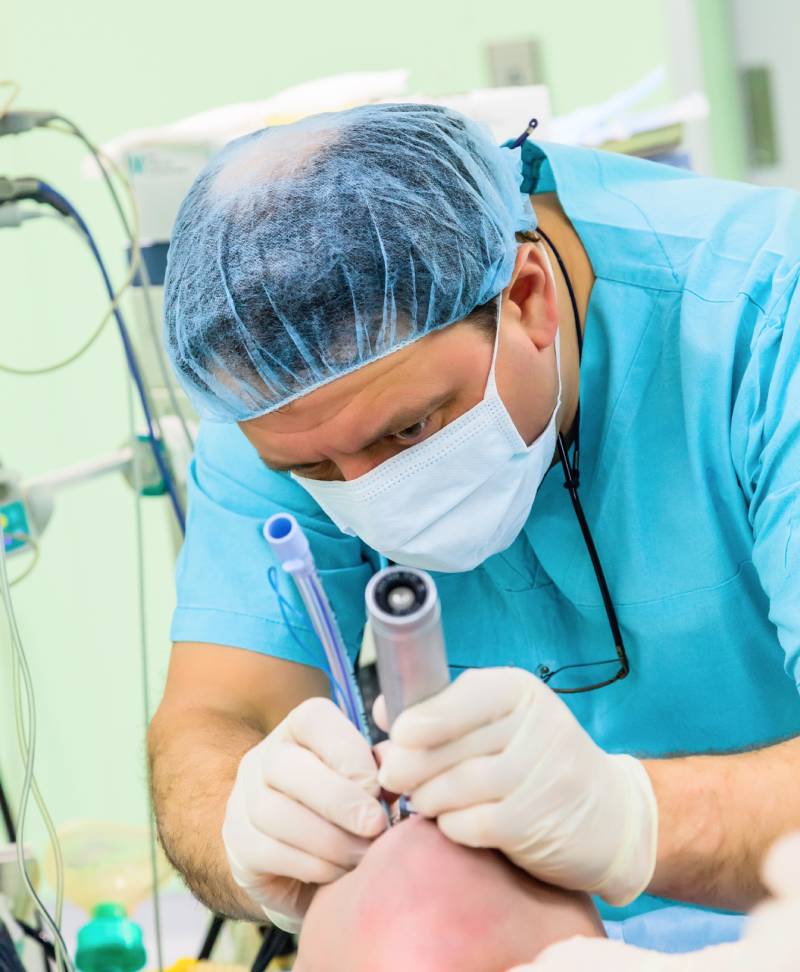
Intubating patients with a swollen tongue is a recognized challenge in airway management. The tongue normally occupies most of the oral cavity, yet it leaves enough space for air movement and visualization of the laryngeal inlet during laryngoscopy. However, when the tongue becomes enlarged due to angioedema, trauma, infection, prolonged positioning, or drug reactions, the posterior tongue can narrow the oropharyngeal space, obstructing both airflow and visualization. A swollen tongue increases the likelihood of difficult intubation and requires modification of standard techniques (1).
In patients with a swollen tongue, direct laryngoscopy often fails because the enlarged tissue occupies much of the oral cavity and cannot be easily displaced by the laryngoscope blade. This prevents the usual alignment of airway axes and obscures landmarks such as the epiglottis and vocal cords. Repeated attempts not only fail to improve visualization but also increase the risk of tissue trauma, worsen edema, and accelerate oxygen desaturation. For these reasons, significant tongue swelling is recognized as a strong predictor of a difficult airway (2).
Advanced devices and techniques are often required when tongue swelling limits the effectiveness of direct laryngoscopy. Fiberoptic intubation, especially when performed while the patient is awake and breathing spontaneously, allows the operator to navigate around a swollen tongue and directly visualize the glottis without relying on a straight line of sight. Video laryngoscopes, such as the GlideScope or C-MAC, offer a similar advantage by providing an indirect camera view that remains useful even when the tongue obstructs direct visualization. Current difficult airway guidelines recommend both techniques as preferred options when standard laryngoscopy is unreliable (3).
In urgent situations, comprehensive protocols and technical skills are essential because a successful first attempt is linked to fewer complications. If intubation fails, clinicians may insert a temporary airway device that sits above the vocal cords, such as a laryngeal mask airway. While these devices can provide short-term oxygenation and ventilation, they do not fully protect against aspiration of gastric contents. When swelling is so severe that neither intubation nor ventilation is possible, creating a surgical airway via cricothyrotomy or tracheostomy becomes the only option. The American Society of Anesthesiologists and the Difficult Airway Society both emphasize that teams should prepare for this possibility before attempting intubation on patients with significant tongue swelling (3).
Both the cause of tongue swelling and patient characteristics influence how the airway is managed once it has been secured. In cases of angioedema, particularly those related to ACE inhibitors, medications such as corticosteroids, antihistamines, and epinephrine can reduce swelling. However, these treatments are too slow to replace the need for immediate airway control. Swelling from trauma or prolonged positioning can last for days, necessitating extended intubation. Planning for extubation is equally important because removing the tube before the edema resolves can lead to sudden obstruction and difficult reintubation (4). Predictors of difficult intubation, such as obesity, pregnancy, limited mouth opening, and a high Mallampati score, can further increase the risk when acute swelling is present. Recognizing these factors allows clinicians to prepare appropriately with preoxygenation, optimal positioning, and the use of advanced devices when needed.
References
- Miller RD, Cohen NH, Eriksson LI, et al. Miller’s Anesthesia. 9th ed. Philadelphia, PA: Elsevier; 2020.
- Apfelbaum JL, Hagberg CA, Caplan RA, et al. Practice guidelines for management of the difficult airway: an updated report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology. 2013;118(2):251-270. doi:10.1097/ALN.0b013e31827773b2
- Frerk C, Mitchell VS, McNarry AF, et al. Difficult Airway Society 2015 guidelines for management of unanticipated difficult intubation in adults. Br J Anaesth. 2015;115(6):827-848. doi:10.1093/bja/aev371
- Walls RM, Hwang J, Murphy MF. Manual of Emergency Airway Management. 5th ed. Philadelphia, PA: Wolters Kluwer; 2018.